Chapter 3: Table of contents
Drains:
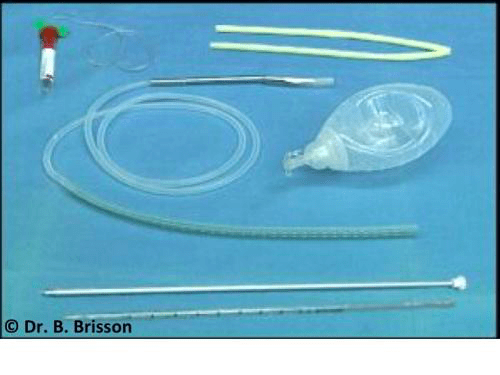
Dead space should be eliminated prior to wound closure to prevent the space filling with fluid resulting in a seroma. Dead space can be eliminated using tacking sutures and bandaging. Drains can also be implanted to prevent fluid accumulation in a space or potential space as they allow evacuation of potentially harmful fluids and help to maintain contact between tissue planes.
Drains can provide active or passive drainage:
-To an area with dead space that cannot be sutured
-To an area of pre-existing fluid accumulation
-To tissue that will continue to secrete fluid
-After wound closure if the tissues are not completely normal (inflammation, contamination, etc.)
Gravity Drains:

Penrose drains are flexible, soft tubes made of Latex. These flat drains are commonly used in veterinary medicine because they are effective and inexpensive. Penrose drains provide passive drainage by capillary action, gravity, and pressure differentials working on the outer surface of the drain (i.e. wound fluid will flow along the outside of the drain with gravity). Other passive drains include silastic or polypropelene tubing.
Penrose Drain Placement:
1. Clip liberally and aseptically prepare the surrounding skin to prevent contamination of the drain exit site by hair or contaminated surrounding skin (bacteria can enter the wound along the drain resulting in an ascending infection.
2. Use as few drains as possible. Drains are foreign bodies and although they might improve drainage and prevent post-operative complications they will incite a foreign body reaction and can decrease wound healing and resistance to infection.
3. Do not exit drains through the primary skin incision or wound as drains incite an inflammatory reaction which could delay wound healing. Drains should exit through a separate stab incision. The stab incision should be large enough to accommodate fluid drainage on the outside of the drain. Typically, the drain is sutured at the exit point using a loose loop of non-absorbable suture.
4. Exit the drain at the most ventral aspect of the dead space (in the most dependent location) to promote passive / gravity drainage.
5. Do not exit the proximal portion of the drain, it should remain under the skin to prevent bacteria entering the wound; Penrose drains are not typically used for flushing. The proximal tip of the drain can be anchored in the wound using a single penetrating suture that passes from the skin surface through the drain and out again to be tied on the outside of the skin. These sutures must be removed to allow drain removal.
6. Do not fenestrate (make holes) the drain as this will decrease the surface area of the drain and decrease it”s effectiveness (drainage occurs by capillary action on the outer surface of the drain).
7. Do not inadvertently include the drain in the subcutaneous suture line or other tacking sutures as this will preclude easy removal and could lead to a piece of drain being left behind.
8. Always bandage the drain (ideally using a sterile dressing) to prevent contamination of the wound by ascending infection or early removal by the patient. Bandaging will also allow to monitor drainage (quality and quantity) and will prevent soiling of the environment.
9. Drains should be removed as soon as they are no longer required to limit the inflammatory reaction and prevent ascending infection.
Penrose Drain Removal:
Drains are typically removed when fluid production has decreased significantly. Most drains are ready to be removed within 3-4 days of implantation. Remember that drainage will never fully cease because the drain will incite a foreign body reaction. Drain related fluid production in the wound generally ranges from 1 to 2 ml/kg/day. Evidence that the fluid has changed from a viscous fluid to a thin, serosanguinous fluid and improved odour are also considered. Significant drainage for longer than 5 to 7 days usually indicates a problem within the wound such as a focus of necrotic tissue, foreign body or resistant infection. Continued drainage from a wound is indication for further surgery to explore, culture, debride and clean the wound.
Closed Suction Drains:
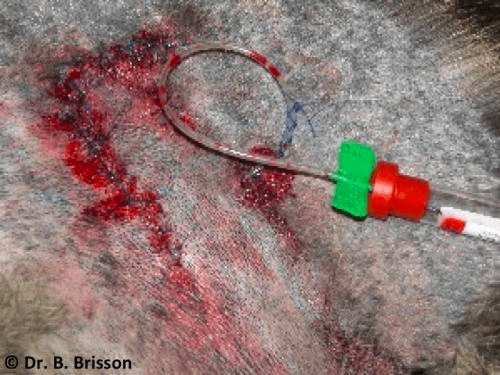
Active or closed suction drains apply negative pressure (suction / vacuum) within a wound to promote fluid drainage and collapse of a wound or potential space. The negative pressure produced by these drains is not sufficient to cause tissue trauma. Active drainage occurs through the lumen of the drain into a closed collection system; allowing accurate assessment of wound drainage fluid. Suction drains are useful when large amounts of fluid are anticipated or when drains have to be placed in an area that is not easily bandaged (e.g. hip area). Closed suction drains are less likely to become infected because the fluid is collected in a closed system (there is no direct contact between the environment or skin and the wound) and the constant negative pressure in the wound prevents retrograde infection. Certain drainage systems are not equipped with a one-way valve and may allow fluid to flow back into the wound when the collection system is disconnected (for emptying) or the patient lies on it.
Closed suction drainage systems include home made systems constructed from large bore butterfly catheters (19 gauge) and a red top blood collection tubes or syringes and more expensive ready to use commercial systems such as the Tuzik® drain (grenade) or Portovac® drain.
Active drains are typically fenestrated in multiple areas along the portion of the drain that remains within the wound to prevent occlusion of all drain pores by tissues or debris. Fenestrations should not be placed too close to the skin exit point as this may result in room air entering the suction system. When making active drains using butterfly catheters, oval fenestrations should be limited to approximately 30% of the diameter of the tubing to prevent kinking and breakage at the time of removal. Active drains can become occluded by debris especially if suction is not applied constantly.
Butterfly with Redtop Tube:

Active suction drains can be constructed using a butterfly catheter and a red top blood collection tube. The luer-lock adapter of the drain is removed and fenestrations are made in the tube portion of the butterfly catheter along a desired length. The drain is inserted through a stab incision close to the wound (active drains do not require to exit in the most dependent portion of a wound like passive drains) and placed in the space to be drained. The drain is typically anchored to the skin at the exit point using a purse string and a Chinese finger trap suture. A 5 or 10 ml red top blood collection tube can then be connected to the needle-end of the butterfly catheter to provide negative suction. Because of the smaller size of the collection system, these home-made drains are useful for small spaces or when only small amounts of drainage are expected. Red top tubes should be changed at least every few hours (even if the tube does not appear full) to prevent obstruction of the drain or loss of vacuum.
Another option is to use a butterfly catheter to construct a drain and a syringe of desired size as a collection system. In this case, the needle end of the butterfly catheter is severed and fenestrations are created along the drain tube. The drain is inserted in the wound and attached to a syringe using the luer-lock adapter. The plunger of the syringe can then be pulled back to create the desired pressure and is anchored in place using a pin or needle.
Commercial Drains:
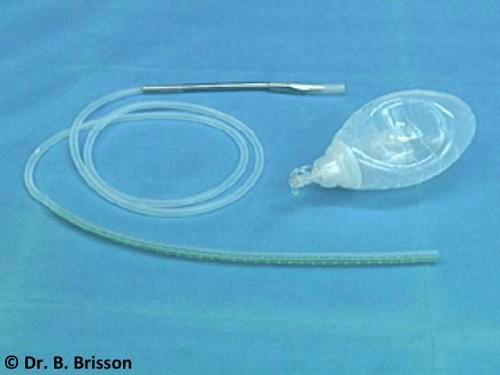
Several commercial, ready to use, closed suction drainage systems are available. Tuzik® (grenade) and Portovac® drains are most commonly used at this institution. These systems include large drains with a high number of fenestrations and large collection systems that are advantageous when draining highly productive cavities such as the abdomen or large wounds. Collection systems are available in various sizes and should also be proportionate to the size of the patient to allow the collection system to be attached to the patient and be portable.
Thoracic Drains:

Any type of firm sterile tubing can be used as a chest drain in case of emergency (red rubber tube, silastic tube, endotracheal tube, etc.). However, commercially available polyvinyl chloride thoracic catheters are preferred. The ideal thoracic drain should not collapse under negative pressure but should be soft enough to prevent lung damage when in place. The diameter of the tube should be sufficient to allow easy flow of air or fluid and prevent obstruction. Side fenestrations can also be added prior to insertion to prevent obstruction and improve flow rate. Fenestrations should be no larger than 30% of the diameter of the tube to prevent kinking and weakening of the tube at that level. Commercial thoracic tubes typically have a radiopaque line that runs along the length of the tube allowing easy radiographic visualization. When creating new fenestrations, the most proximal fenestration (farthest from the tip) should be created along the radiopaque line to allow radiographic identification of the last hole as a break in the radiopaque line. The most proximal hole should not be located too close to the skin entry point as this could allow room air to enter the thoracic cavity.
Thoracic drains are maintained using a closed system to promote negative pleural pressure. Thoracic drainage can be intermittent or continuous depending on the situation. Intermittent drainage is usually safer, less cumbersome and more convenient. Continuous drainage is typically required with tension pneumothorax or when high volumes of air and/or fluid are produced. The negative pressure applied to the drainage system must not exceed 30 cm H2O to prevent lung injury and obstruction of the fenestrations by mediastinal tissue.
Just like drains placed in wounds, thoracic drains produce a foreign body reaction that results in fluid production. Normal drain-related fluid production ranges from 1 to 2 ml/kg per day. Drain removal usually occurs when no air is produced for 12 to 24 hours and/or fluid production has decreased to the normal drain related volume. The drain can be clamped and left in place for another 12-24 hours without drainage to ensure that removal is appropriate. Drains are removed using rapid traction and the skin incision is sutured, stapled or left open and covered with ointment and a bandage for a few days to allow formation of a seal.
One Way Valve:
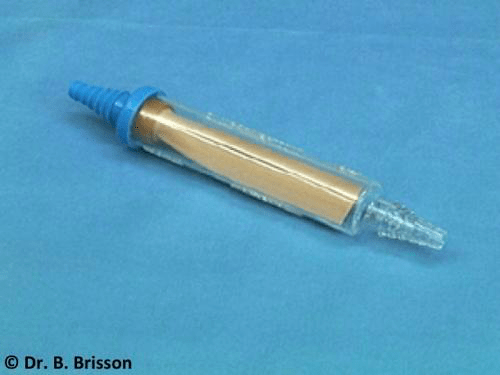
A one-way valve or Heimlich chest drain valve can be used for continuous drainage of the chest. This valve is attached to the end of the thoracic tube; it allows air and fluid to exit the chest on exhalation. The valve does not allow any air to enter the chest, enabling the patient to develop negative pressure for lung expansion. A one-way valve requires adequate expiratory pressure to function properly. Many small dogs and cats do not exert enough pressure, nor do painful dogs taking shallow breaths, reducing its usefulness in veterinary medicine.
The one-way valve can allow for greater mobility (vs. continuous suction) if the animal needs to be moved throughout the facility. Any animal with a thoracic drain should be monitored 24 hours a day and despite the greater mobility offered by this valve, it does not reduce the need for careful observation.
Hemostatic Agents:
When attempting to control surgical hemorrhage, bone wax and synthetic materials made with gelatin or cellulose may be used.
Gelofoam®:

Gelfoam® is an absorbable gelatin sponge that can be applied to areas of hemorrhage where it will absorb blood, will swell and exert pressure to produce hemostasis. Gelfoam® is absorbed (over 4-6 weeks) better than bone wax but should be removed if possible as it may promote infection, granuloma formation and in bone, may slow or prevent healing. Granuloma formation has been reported when used in the brain.
Bone Wax:

Bone wax is made of synthetic beeswax and a softening agent (isopropyl palmitate). When applied it inhibits bleeding by filling the vascular cavities and pores in the bone. It should be used sparingly as it may prevent healing, it may promote infection and remains in the tissues for years after implantation.
Instat®:
Instat® is made of purified and lyophilized bovine dermal collagen. It allows platelet aggregation to form a fibrin clot. It may also potentiate infection when bacterial contamination is present.
Surgicel®:

SURGICEL® is an oxidized regenerated cellulose fabric that activates clotting when it contacts blood (not with other fluids). It should also be removed if possible after bleeding is controlled as it may promote infection. This product may have antibacterial effects in vitro.
Fibrin Glue:
Fibrin glue may be useful to control paranchymal bleeding e.g. liver and splenic hemorrhage and can be useful in patients with coagulopathies.


