Chapter 22: Table of Contents
Surgeries of the Upper Urinary Tract
Nephroliths and ureteroliths are frequently identified in dogs and cats. Though nephroliths are not typically a condition that requires intervention, ureteral obstruction represents a challenging and often emergent condition for which medical management is rarely successful. Ureteral obstruction may be caused by the presence of calculi, blood clots/blood stones, mucous plugs and debris, stricture, and more rarely neoplasia or external compression. In cats, most obstructions are caused by calculi (nephroliths that have migrated or fragmented), blood stones or stricture. (Kyles 2005) 98% of feline and over 50% of canine ureteroliths are reportedly calcium oxalate. (Kyles 2005).
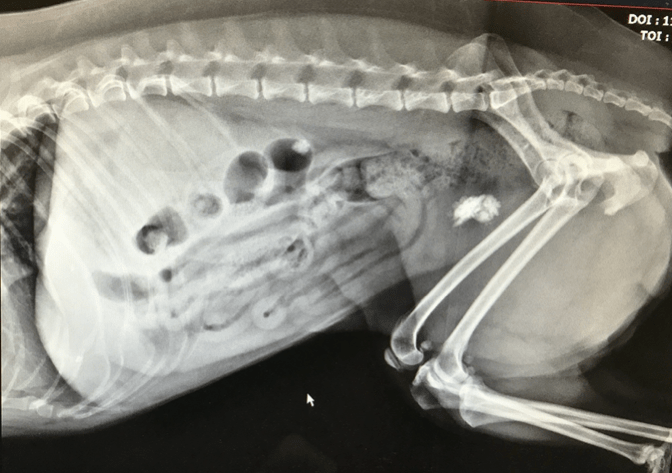
The normal ureteral diameter of the cat measures 0.4mm and that of the dog 1.3-2.7 mm. (Berent 2011) As such, stones as small as a few mm in diameter can cause intermittent, partial or complete obstruction or even lead to stricture after passing into the urinary bladder. In dogs, ureteral obstruction leads to loss of renal function (GFR) quite rapidly and is reported to be permanently diminished by a mean of 35% after 7 days of obstruction. (Fink et al. 1980) If relieved within 4 days, the damage appears reversible but if left untreated for 14 days or more, at least 50% of the renal function will be lost permanently and after 40 days of obstruction the kidney will have lost almost 100% of its function permanently. (Wilson 1977)
Unilateral obstructions are more common (Kyles 2005) but often go undiagnosed due to the overall sufficient contralateral renal function leading to clinical signs once one kidney is already compromised if the second kidney also becomes compromised.
Diagnosis is typically based on ultrasound findings but it is important to note that obstruction can exist without the presence of renal pelvis dilation (especially in cats) and that sometimes it can only confirmed with pyeloureterogram under fluoroscopic guidance.
The majority of ureteral obstructions are caused by calculi that cannot be dissolved medically and require relatively emergent treatment in order to relieve the obstruction leaving medical and surgical options available. The mainstay of medical management for ureteral obstruction includes aggressive fluid therapy (based on hydration status and ability to handle fluid therapy), analgesia, and drugs aimed at relaxing the ureter by dilating it and relieving spasm (e.g. prazocin and tamsulosin) with the hope of facilitating the passage of obstructive calculi. Despite appropriate treatment, only 8-17% of cases appear to respond positively with some movement of the calculi. (Kyles 2005) In addition, since 62% of cats were shown to have concurrent nephrolitiasis, the medical passage of ureteral calculi is only temporary and often followed by re-obstruction. 1 year survival for cats treated medically was ~62% vs ~91% for cats treated surgically (Kyles 2005) with 14/35 cats having recurrence of ureteral obstruction within 12 months.
Surgical options consisting of ureterotomy, ureteronephrectomy, neoureterocystostomy (for very distally located stones) are highly complex and associated with a guarded to poor prognosis relating to the high complication and mortality rates. These procedures require advanced surgical skills and in some cases magnification. Complications associated with ureteral surgery include: difficulty localizing the obstructive stone/stricture, dehiscence and leakage leading to uroabdomen, postoperative stricture, and continued or recurrent obstruction. Perioperative mortality rates reported for ureteral surgery range from 18-39%, which is considered unacceptably high since novel alternatives now exist.
Less invasive surgical / interventional options such as ureteral stenting and subcutaneous ureteral bypass have been described and are now considered standard of care for ureteral obstructions that are not good candidates for standard surgery.
< Prognosis Ureteral Stenting >
Reference:
Berent AC. Ureteral obstructions in dogs and cats: a review of traditional and new interventional diagnostics and therapeutic options. J Vet Em Crit Care 2011; 21:86-103.
Kyle AE, Hardie EM, Wooden BG et al. Clinical, clincopathologic, radiographic, and ultrasonographic abnormalities in cats with ureteral calculi: 163 cases (1984-2002). JAVMA 2005; 226:932-936.
Fink RL, Caradis DT, Chmiel R, et al. Renal impairment and its reversibility following variable periods of complete ureteric obstruction. Aust N Z J Surger. 1980; 50:77-83.
Wilson DR. Renal function during and following obstruction. Ann Rev Med. 1977; 28:329-339.


