Chapter 21: Table of Contents
Prognosis
Although tracheal stenting provides a minimally invasive approach to treating tracheal collapse therefore avoiding several of the complications encountered with extraluminal stenting, complications associated with the presence of a foreign body within the lumen of the trachea are clearly present. Reported success rates vary from 75-90%. Most complications were minor including coughing, tracheal hemorrhage and pneumomediastinum. Perioperative mortality rates of approximately 10% have been reported due to aspiration pneumonia, worsening of clinical signs and incorrect stent placement. In my experience, dogs that present intubated, that cannot tolerate extubation prior to stenting and have aspiration pneumonia have a higher mortality rate than dogs undergoing an elective stenting but many will still fare well. Reported long-term complications include stent migration (if too small a stent is implanted), excessive granulation tissue formation (20-30% of cases and typically responds to steroid therapy), stent shortening (as the stent expands to reach its predetermined diameter) which can result in collapse beyond the stented area, stent fracture, and progressive tracheal collapse beyond the stented area (due to progression of disease). Pneumonia and recurrent bacterial tracheitis can occur intermittently and is reportedly more likely if a gap exists between the stent and the trachea.
The main complication I have encountered is persistent coughing. The stertour, honking cough, wheezing, cyanosis, exercise intolerance, and syncope stop immediately after stenting. However, coughing is significant for at least 3-4 weeks after stenting and for some dogs it seems to persist long-term. I have found that dogs that cough are often in smoking households, have mainstem bronchus collapse or their stent is very close to the carina or cricoid. Persistent coughing after stenting is a serious issue since repetitive coughing could lead to stent fracture. For this reason, all dogs undergoing intraluminal stenting should continue to receive a cough suppressant (e.g. hydrocodone) for life. I typically also continue the tracheal elixir, at least for the first few months and prescribe a tapering dose of prednisone for at least one-month post stenting and then as needed for severe episodes of cough. Some dogs cannot be weaned of steroids and some can but eventually require it to be added again. Broad-spectrum antibiotic therapy is recommend for 2-4 weeks after the procedure to prevent infection around the implant. If tracheoscopy was performed, antibiotic therapy is adjusted based on bacterial culture results once they are available. Episodes of worsened cough are likely to occur once or twice a year and typically around the change of season (fall and spring). These usually respond to a course of antibiotics and increased steroid therapy. Adjustments (up and or down) in hydrocodone and steroid doses may be required over time. Owners should be advised that tracheal stenting is a palliative procedure. Most owners are amazed at how incredibly well their pet is doing after stenting. Tracheal stenting can improve respiratory function and quality of life for months to years but will unfortunately not prevent progression of disease. Collapse beyond the stented area is possible and could require further stenting in the future.
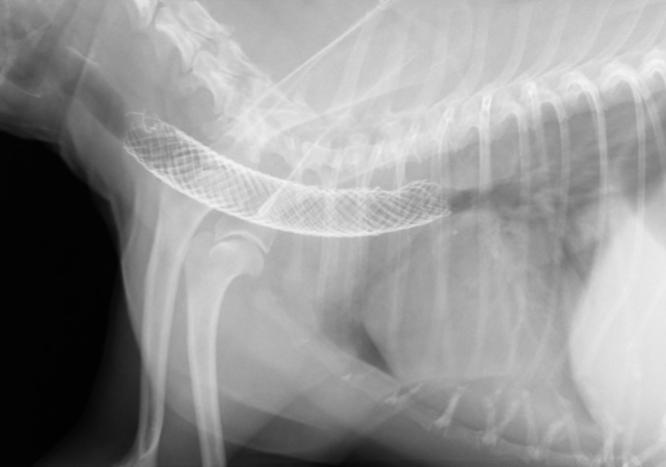
Dogs with mainstem bronchus collapse may still benefit from tracheal stenting but owners should be warned that improvement may not be as dramatic. Tracheal stenting has changed the way we treat severe and non-responsive tracheal collapse. The main disadvantages of intraluminal stenting include the need for advanced training, access to fluoroscopy and the fact that stents are relatively expensive. Owners should however realize that regular radiographic reassessments (every 3 months the first year and every 6-12 months thereafter unless issues arise) with continued life-long medical management will be necessary following tracheal stenting.
< Intraluminal Tracheal Stenting Surgeries of the Upper Urinary Tract >


