Chapter 18: Table of Contents
Rhinoplasty for Stenotic Nares
Stenotic nares are narrower than normal and also can tend to collapse during inspiration further obstructing the flow of air through the nasal cavities. The goal of rhinoplasty is to enlarge the nare opening by removing a portion of the malformed dorsolateral cartilage to increase air flow.
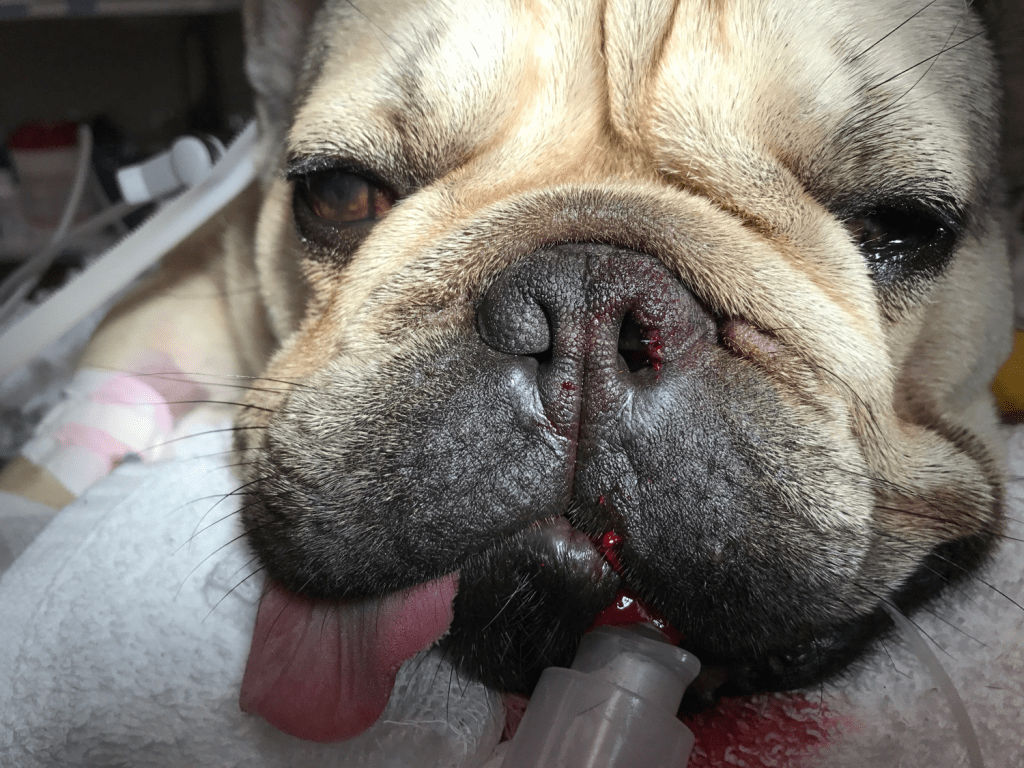
Various procedures have been described for rhinoplasty including wedge resection, biopsy punch resection, laser resection. The procedure I like best is the pyramidal wedge resection with sutures.
First, I ensure the patient’s head is appropriately positioned (straight) with towel support under the chin and the mouth closed. I usually tape the head to the table to ensure the patient’s head does not move.
The left nostril is easier for a right-handed surgeon and so I typically start there. With Debakey or Adson tissue forceps, I grasp the ventro-lateral free edge of the nare and pull it medially. Using a #11 blade, I make a first cut along the medial aspect of my proposed wedge (just adjacent to where I am grasping the free edge). This cut is made vertically. The blade must penetrate the nare quite a ways to ensure a proper wedge is created. Bleeding will immediately obstruct the field. Don’t let go of your tissue bite and make your second cut on the lateral aspect of the tissue removing the wedge of tissue. This second cut is made at a 45 degree angle (dorsomedial to ventrolateral). Release the ventro-medial edge, dab and get ready to suture the edges back together. The first interrupted suture (4-0 Monocryl) is placed at the most ventral aspect of the tissues to ensure proper apposition of the tissues. Once this first suture is in place, bleeding will subside markedly. Before placing any more sutures, assess the opening and determine if more tissue should be removed. If more tissue should be resected, remove the single suture placed and resect further tissue from the lateral margin of the gap (this will not be easy!). Then suture again. Typically, 2 or 3 simple interrupted sutures are placed; one at the most ventral border (edge of tissue), one above and sometimes one suture is required inside the nostril to stop deeper bleeding. Suture ends are cut short to prevent irritation.
Repeat the procedure on the opposite side ensuring that the nostrils are as symmetrical as possible. Note that in many cases, rhinoplasty exposes pink nasal mucosa so the owners should expect that this may be the case.
Excessive nasopharyngeal turbinates have been identified as a cause of upper airway obstruction in certain breeds and some believe that this should be corrected in order to significantly improve the upper airway obstruction. Laser assisted turbinectomy (LATE) procedure has been described and is more commonly performed in Europe at this time. (Schuenemann 2014 and 2017, Oechtering 2016)
An Elizabethan collar is essential postoperatively to prevent self-trauma. An attempt can be made to remove the external sutures after 10-14 days but in most cases the patient is not very cooperative and the sutures will fall on their own.
Note that patients undergoing airway examination for intervention at an early
age, may not yet have everted saccules (secondary change). In this case, sacculectomy is not
possible. If the remainder of the
abnormalities (palate and/or nares) are corrected, reducing excessive upper
airway pressure, it is possible the saccules will never go on to evert. However, I always warn owners that it is
possible for the saccules to evert in the future and for their pet to become
acutely clinical and require an additional short procedure to remove them at
that time.
Postoperative care includes continuous monitoring, continued administration of metoclopramide and sometimes antibiotics (if aspiration is suspected or confirmed), analgesics and possibly sedatives as well oxygen supplementation as required. Dexamethasone (0.25 mg/kg) is administered to dogs with severe laryngeal swelling and expected poor anesthetic recovery (unless otherwise contraindicated). In rare instances, tracheal intubation and mechanical ventilation or temporary tracheostomy is required. If a steroid was not required, a NSAID such as meloxicam can be administered after the initial recovery.
The most common complication is typically dyspnea related to upper airway swelling and inflammation; this may be severe enough to require re-intubation. For this reason, older dogs who are expected to have more severe secondary changes should be sent to a referral center when possible for surgery and postoperative monitoring in an ICU.
Permanent tracheostomy may be required in patients that have severe laryngeal collapse, markedly hyperplastic pharyngeal tissues and do not respond to standard surgical intervention. Managing a permanent tracheostomy site can be challenging in breeds with excessive cervical cutaneous folds and is not for every owner.
Postoperative expectations should be realistic. We can improve the airway but the dogs remain brachycephalic! Though most owners report a significant improvement in clinical signs postoperatively, dogs typically continue to snore during sleep and show signs of stridor / stertor when conscious. (Torrez 2006) In one study, most dogs (84%) with laryngeal collapse responded well to surgery. (Torrez 2006) In another study, the presence of hypoplastic trachea did not affect outome in dogs undergoing surgery. (Riecks 2007)
Reported complications following brachycephalic surgery include airway swelling and inability to extubate, regurgitation and aspiration pneumonia, dehiscence of nare and or palate resection sites, voice change and pharyngeal scarring due to excessive trauma related to the sacculectomy, and persistent upper airway signs
< Normal Laryngeal Function Laparoscopic Ovariectomy >
References
Oechtering GU, Pohl S, Schlueter C, Schuenemann R. A Novel Approach to Brachycephalic Syndrome. 2. Laser-Assisted Turbinectomy (LATE). Vet Surg. 2016 Feb;45(2):173-81.
Riecks TW, Birchard SJ, Stephens JA. Surgical correction of brachycephalic syndrome in dogs: 62 cases (1991-2004). J Am Vet Med Assoc. 2007 May 1;230(9):1324-8
Schuenemann R, Oechtering G. Inside the brachycephalic nose: conchal regrowth and mucosal contact points after laser-assisted turbinectomy. J Am Anim Hosp Assoc. 2014 Jul-Aug;50(4):237-246.
Schuenemann R, Pohl S, Oechtering GU. A novel approach to brachycephalic syndrome. 3. Isolated laser-assisted turbinectomy of caudal aberrant turbinates (CAT LATE). Vet Surg. 2017 Jan;46(1):32-38.
Torrez CV, Hunt GB. Results of surgical correction of abnormalities associated with brachycephalic airway obstruction syndrome in dogs in Australia. J Small Anim Pract. 2006 Mar;47(3):150-4.


